|
Just three weeks after George Floyd’s murder, 26 year-old Sha-Asia Semple died shortly after the birth of her first child due to fatal errors in properly administering her epidural and a subsequent failed intubation in a Brooklyn public hospital. In September of 2021 in Queens, NY 29 year-old mother of two Denise Williams died 48 hours after being admitted to the hospital for complaints of postpartum depression. Although at first the cause of her death was unknown, later reports confirmed it was a pulmonary embolism that had gone undetected. According to her family, Ms. Williams had been under enormous physical and emotional stress during her two month postpartum period, but hadn’t been able to address her own health needs until it was too late.
Although seemingly unrelated incidents, both cases involved the untimely death of two black mothers in NYC related to huge disparities in our maternal healthcare system. In New York City, Black women are nine times more likely to die of pregnancy-related complications than white women. Research suggests that racial disparities in maternal deaths are also linked to the fact that Black women are often more likely to deliver at hospitals with a lower quality of obstetric care, ranging from lower-performing doctors to understaffing, which forces patients in distress to wait longer. This breeds negligence and incompetence, making tragic but preventable cases like Sha-Asia and Denise’s more common. In a post-Roe America, there are more barriers than ever preventing black birthing people from getting the critical perinatal care they deserve, including lack of paid parental leave as well as lack of insurance coverage for postpartum doula care or mental and behavioral health care for PMADs, (approximately 80% of which go undetected due to lack of awareness, routine screening, and stigma.) The words of Shawnee Benton Gibson, whose daughter Shamony Gibson also died from a preventable pulmonary embolism in 2019, echo louder than ever: “Black wombs matter. Black minds matter. Black bodies matter. Black communities matter.” Post by Sharon Itkoff Nacache ATR-BC LCAT LPAT PMH-C Original photo via Unsplash
0 Comments
A recent "Discover" magazine article highlighted the benefits of visual art exposure on mental health. Viewing visual art activates the same brain reward systems as other pleasurable, highly sensory activities. Studies have shown that regardless of the context of where the art is observed–whether it's a gallery, museum, or even an online exhibit from home–other physiological benefits can include lowered stress levels, blood pressure, and anxiety when engaged in mindful art observation for at least two minutes. “Maybe it makes you think about your identity, evokes certain memories or elicits different sensations. This may allow you to learn new things about yourself and make the art-viewing experience something transformative,” reflects art therapist Sarah Vollmann. Imagine if this positive impact could be translated to stressful workplace environments as well. Particularly for those in “frontline” helping professions during the ongoing pandemic, caregiver burnout remains an underreported yet incredibly common mental health syndrome exacerbated by lack of systemic support and exposure to chronic stress. This can lead employees to feel “checked out,” undervalued, resentful, and/or reactive, which in turn, negatively impacts job performance and quality of patient care. In response, the Whitney Museum of American Art has recently partnered with NYC Health + Hospitals Arts in Medicine program to provide integrative arts-based wellness workshops to hospital employees inspired by art pieces on loan from their collection and featured throughout the medical facility. Yesterday I was privileged to begin a new role in co-facilitating the first of these integrative workshops at a Manhattan hospital, where we applied creative resilience skill-building, social-emotional learning, and art observation mindfulness techniques to creative responses pieces and personal reflection. Vollmann continues, “I believe that the importance of art cannot be overstated. We are living in difficult times, and struggles with mental health are on the rise. The exhibits of museums and galleries can provide a sanctuary of sorts from the chaos and stress of our daily lived experiences, and, conversely, they can help us to face and make meaning of the struggles that we face.” Now, through this program, we are working to bring these crucial creative safe spaces to the workplace as well. #burnoutprevention #caregiverburnout #mentalhealthawareness #artheals #creativeresilience #mindfulness #safespaces Post, artwork, and photograph by Sharon Itkoff Nacache ATR-BC LCAT LPAT PMH-C   “I think this is me,” one of my best mom friends sent to me with a hand smacking face emoji and a link to a recent “Parents” magazine article entitled “How the Snowplow Parenting Trend Affects Kids.” My friend, I may add, happens to be a brilliant early childhood educator and BIPOC identifying military solo parent of two highly sensitive boys, not unlike my own. I skimmed the article, citing various parenting experts and mental health professionals and listing the negative effects of overprotecting our children–including low frustration tolerance, poor problem solving skills, learned helplessness, and high anxiety. Although, in theory, I agree that children need to learn experientially by trial and error so that they can better cope with distress in the future and that parents shouldn’t “hover” or overly interfere with their children’s every concern, I fundamentally disagree with the covert parent-shaming that is often the subtext of these parenting buzzwords that have become mainstream, like “snowplow parent, lawnmower parent, helicopter parent, tiger mom,” etc. etc. Pediatrician and child psychoanalyst D.W. Winnicott coined the term “good enough mother” in the 1950's to challenge archetypes around the “perfect,” saintly, martyr-like mother or the now debunked “refrigerator mother” stereotype. His theory posits that in order to be a “good enough” parent and ensure an infant’s healthy biopsychosocial development, parents must do a delicate balancing act that alternates between attuning to their every need while also allowing for a degree of frustration to encourage self-soothing and begin a healthy path toward autonomy. To me, this continues to be a parenting model worthy of striving toward. As a pandemic parent specializing in perinatal mental health, I can say from personal and professional experience that today’s parents are under more strain and scrutiny than ever. Add to the mix the maddening impact of social comparison via social media, ongoing maternal mental health crisis, overturning of Roe v. Wade compromising our basic reproductive rights, the devastatingly high black maternal mortality rate, and school shootings on almost a monthly basis in this country, and it becomes almost a cruel joke when we ask our parents to “back off” and “relax.” Hypervigilance and protecting our young is evolutionary and adaptive, and instead of pathologizing and mocking the unique challenges of parenting in this age of anxiety and maintaining our own mental health at the same time, why not offer up some solidarity, validation, or compassion? Wherever you fall on the spectrum of protecting our most vulnerable, trust that it is not only “good enough” but that society at large needs to do better in both recognizing and supporting that. Post by Sharon Itkoff Nacache ATR-BC LCAT LPAT PMH-C Original image by Joy Wang via Unsplash 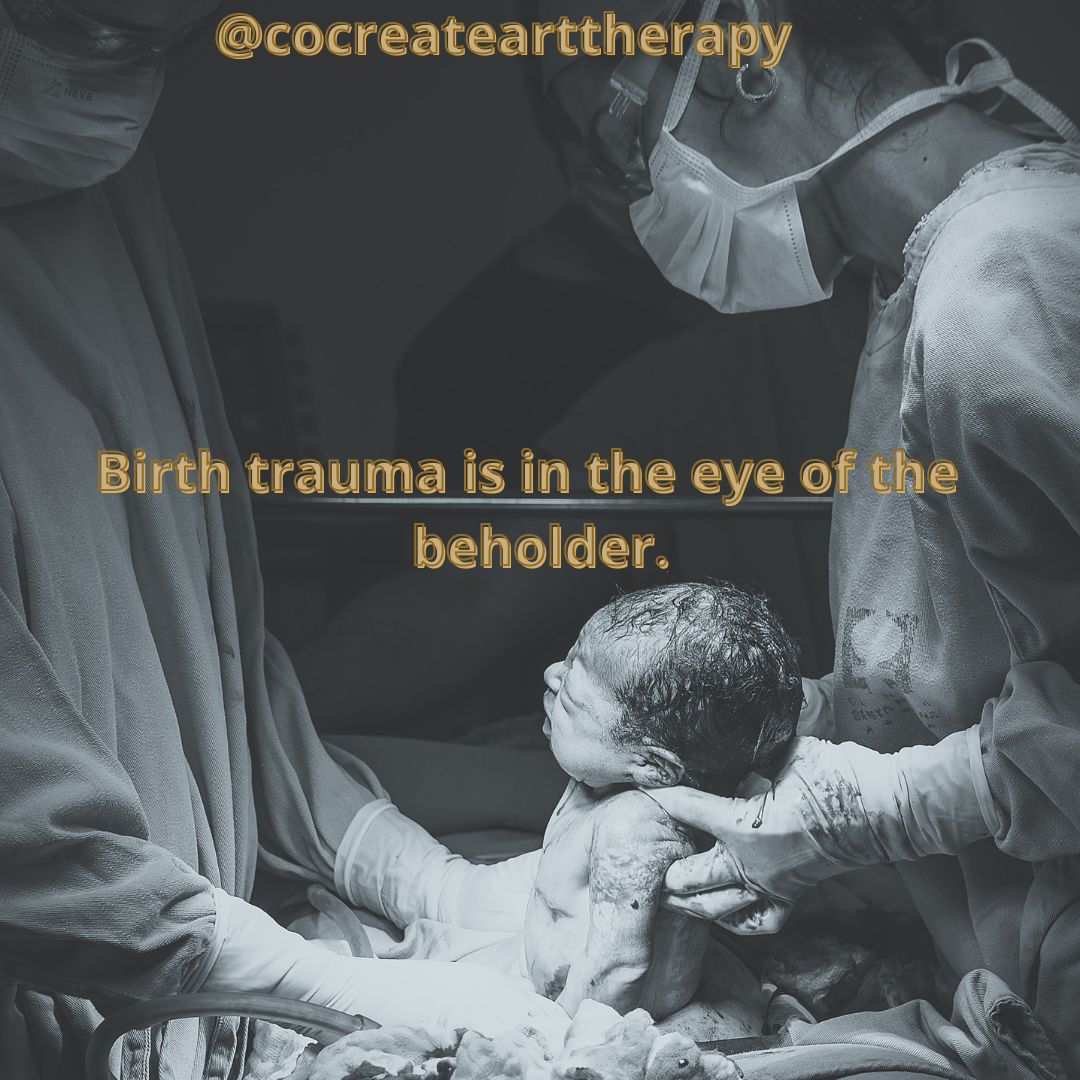 www.youtube.com/watch?v=2dsCmWZ0V_UCheryl Beck (2018) shares that up to 45% of new mothers have reported experiencing birth trauma and adds that “birth trauma is in the eye of the beholder.” Indeed, if a birthing person experiences or perceives that they and/or their baby were in danger of injury or death during childbirth, their birth can be defined as traumatic–psychologically, physically, or both (even if others present may have perceived it as routine.) Common themes present in those who have shared traumatic birth narratives include:
Art-making and creative processing can provide a symbolic container of overwhelming experiences, helping with the reconstruction of fragmented memories and emotional responses. Wolf & King (2020) summarize how art therapy “facilitates the organization and integration of traumatic memories, reactivates positive emotions, serves as a vehicle for exposure and externalization of difficult content, and reduces heightened arousal responses.” Art therapist Swan-Foster (2020) poignantly asks, “What if we viewed pregnancy and birth through a lens of cultural humility and feminism that honors a woman’s desire to have control of herself throughout pregnancy and birth while holding the knowledge that these experiences may be out of control and traumatic?” As trauma is so often stored in the body or in the mind as imagery, art therapy helps to navigate between these polarities and honors the “gray” area of personal experience. Learn more and experience how intuitive artmaking and creative processing can help perinatal professionals and birthing folk creatively cope with trauma experiences at the upcoming virtual conference "Healing Traumatic Birth: Tools and Techniques from Psychodrama, Dance, and the Expressive Arts" via PATTCH. Post by Sharon Itkoff Nacache ATR-BC LCAT LPAT PMH-C Original photo by Patricia Prudente via Unsplash Compassion fatigue and burnout syndrome are real, especially for birth workers, healthcare professionals, parents and professional caregivers who continue to work on the "frontlines" of an ongoing pandemic and maternal mental health crisis. Aside from individual and group therapy, I offer arts-based wellness workshops as a chance for these populations to reconnect with their "inner artists" and immerse themselves in a much needed creative self-care break. No artistic experience is necessary and basic art materials can be used. Here are some mixed media images of artwork I've created during workshops facilitated this fall using an adapted open studio process method. Contact me for more info about upcoming workshops including availability and rates. #selfcare #burnout #compassionfatigue #vicarioustrauma #birthtrauma #grief #birthworkers #pandemic #healthcare #maternalmentalhealth #perinatalmentalhealth #openstudioprocess #arttherapy #perinataltherapist #cocreate #artastherapy #artheals
 Holiday season is always emotionally charged, especially for new parents who are stressed about introducing their new bundles to loved ones, attending first family-friendly social gatherings since emerging from their pregnancy or newborn “bubble,” feeling pressure to host, or trying to present themselves as more “put together” than they actually feel during this massive life stage transition. A recent article from “Self Magazine” reminds us how support for new parents can come in many forms. Alexis Barad-Cutler, mother and director of the maternal advocacy nonprofit called The Chamber of Mothers, advocates, “Helping is not holding the sleeping baby. It means letting the new parent nap, doing laundry, doing dishes, or tidying up.” Indeed, rest and sleep are especially important for a new parent’s recovery and mental well-being. Chronic sleep deprivation can significantly contribute to symptoms of perinatal mood and anxiety disorders for either parent, which is why some savvy baby registries now include “sleep funds” to help new parents afford overnight support such as a baby nurse or postpartum doula. Barad-Cutler believes, “giving new parents the gift of rest is so important to their mental health, recovery, and their relationships.”
But protecting parental sleep is not the only way to offer support. Sending loving texts with no pressure or expectation for a response, having a hot meal delivered to their doorstep, or, most importantly, holding space for however they are adjusting to new parenthood in that moment can all be enormously helpful. It is rare that new parents feel they can reveal the “messiness” around this life stage without guilt, shame, social comparison, or fear of judgment. Paige Bellenbaum, LMSW of The Motherhood Center explains,“We need to give new parents permission to talk about how hard this can be. If we can normalize the hard parts, maybe then we can start to address some of the fundamental needs in this country like adequate and extended paid family leave, subsidized childcare, and better supporting the needs of new and expecting parents.” #newparents #holidayseason #emotionalsupport #postpartum #perinatalmentalhealth #stress #parenting #cocreatearttherapy Post by Sharon Itkoff Nacache ATR-BC LCAT PMH-C Original Photo by Josh Boot via Unsplash  In the 1920s social psychologist Graham Wallas proposed one of the first models of the creative process: preparation, incubation, illumination, and implementation. In the midst of this season of transition, with temperatures fluctuating daily and a kaleidoscope of leaves changing color all around us, it can be helpful to introduce a creative practice into your routine, which can be paralleled with the “preparation” phase before the hibernation/incubation of winter. This can be daunting for those who struggle with seasonal affective disorders, don’t identify with the Artist title, or perhaps have role fatigue and have gotten stuck in a creativity block. Trish Duggan writes in a recent “Rolling Stones” article, “…the need for art does not always strike at the most convenient times. In fact, the need for art may come when you are feeling the least inspired. But it is at these times when it is critical to be intentional about making space for it. From my perspective, art, creativity and imagination are essential to human mental well-being. If you can’t create a lot, create a little.” Indeed, formal art training with traditional art supplies are not necessary for living creatively. Creative personal expression can look like a 10 minute journal doodle, adding a new spice to an old recipe, arranging fruit in an aesthetically pleasing way on the countertop, making a seasonal playlist for friends, improvising a dance to your latest favorite song, engaging your child in imaginative play to help them finish their vegetables, etc. In my clinical opinion, any and all expressions of personal creativity can be therapeutic, especially if it helps you tap into a playful or mindful state. Creating “art for art’s sake” is an exercise of self-care that can cultivate self-compassion and aid in healing. So, whether you resonate with this season of change, dread it, or somewhere in between, finding small daily outlets for your own personal creativity can help you weather it. Post by Sharon Itkoff Nacache ATR-BC LCAT PMH-C Original Photo by Zeynep Sumer Today I had the privilege of chatting live with Lindsey Bliss, doula, mother of 7, and co-founder of Carriage House Birth. We discussed pregnancy anxiety, self care in early postpartum and beyond, parenting stress, creative resilience, idealized motherhood, self compassion and so much more! Check it out!
Perinatal loss impacts 1 in 4 childbearing families. It is estimated that about 10-15% of known pregnancies end in miscarriage. A stillbirth occurs after 28 weeks of pregnancy and before birth, and neonatal death occurs within the first month of birth. About 1 in every 50 pregnancies in the US is ectopic, meaning the egg is fertilized outside of the womb and therefore not viable. Despite these significant statistics of events often experienced as traumatic, unexpected, and life-changing, they are still considered taboo. With the recent overturning of Roe vs. Wade, ALL pregnancies–whether unwanted, ectopic, or medically complicated–are now scrutinized, jeopardizing maternal physical and mental health. Individuals and families experiencing perinatal loss often experience disenfranchised grief since societal expectations for mourning associated with this kind of loss are noticeably absent. Bereaved mothers in particular are more at risk for perinatal mood and anxiety disorders– 4 times more likely to develop depressive symptoms and 7 times more likely to develop PTSD.  TV personality and model Chrissy Teigen has become a recent spokesperson for miscarriage after publicly sharing details of her and husband John Legend’s loss at 20 weeks in utero in 2020. She explained to “People” magazine, “I think that it's important that more people keep talking about it and more people talk about their losses, so people know that they're not alone in all that. Because I think one of the hardest parts about it is you just feel like, 'Am I the only person? Why is it not working for me?' We see these perfect lives and these pregnant bellies and people covered in children. And it could be really frustrating to compare yourself to people that seem to have everything all the time." Health and healing are possible in the face of perinatal loss, especially with social support and sensitive presence, which can buffer the effects of the trauma and reduce isolation. Creating meaning through the sharing of the story of parental loss, engagement in sociocultural rituals associated with loss, creation of tangible mementos, and validation of the loss with peers and trained mental health professionals also promote resilience and post-traumatic growth. If you or someone you love has been impacted by perinatal loss and seeking support, please reach out. Post by Sharon Itkoff Nacache ATR-BC LCAT PMH-C Original Image by Mustafa Omar via Unsplash With school almost back in session and the autumnal equinox around the corner, it's a perfect time to practice self care. Join CBT expert Dr. Terri Bacow, Ph.D and myself virtually on Thursday September 22 from 12-1pm for a free, experiential workshop to learn several concrete coping strategies to reduce daily anxiety and practice mindful art-making for stress management in real-time. All that is needed is basic drawing materials and an open mind! Spaces are limited so register today here.
|







 RSS Feed
RSS Feed